Gabriella Bowling, Towns County High School (Hiawassee, GA)
The act of giving birth is an intense experience – perhaps the most intense experience any woman could have. Not only is labor very physically demanding, but bringing a new child into the world can have a great impact on the new mother’s mental health and wellbeing. Society tends to place heavy emphasis on the health and safety of the infant, which is completely valid in its own right; however, the safety of the mother – as well as the acknowledgement of postpartum/perinatal mental conditions – is often overlooked and invalidated.
HORMONAL INFLUENCE
Throughout pregnancy, various hormones serve different functions that prepare the body for carrying and delivering a child. Human chorionic gonadotropin (hCG) is considered an early hormone active during the first trimester and is responsible for signaling the end of menstruation once an egg fertilizes. In addition, the human placental lactogen (hPL) prepares the body for milk production while providing the fetus essential nutrients via the placenta. These crucial hormones are coupled with rising levels of Progesterone and Estrogen, which gradually prepare the woman’s body for a homeostatic, or healthy pregnancy (Johns Hopkins Medicine, n.d.)1. Upon finally giving birth, the hormones Prolactin and Oxytocin increase to establish milk production and stop uterine bleeding respectively. Simultaneously, Progesterone and Estrogen dramatically plummet after delivery (Hackenstack Meridian Health, 2023)2. Though each serves to ensure the healthy development of a baby, the constant fluctuation in hormonal levels often weigh on the mother’s physical, mental, and emotional capacity. These hormonal shifts, along with other preexisting factors, bring the probability for Perinatal Mood and Anxiety Disorder.
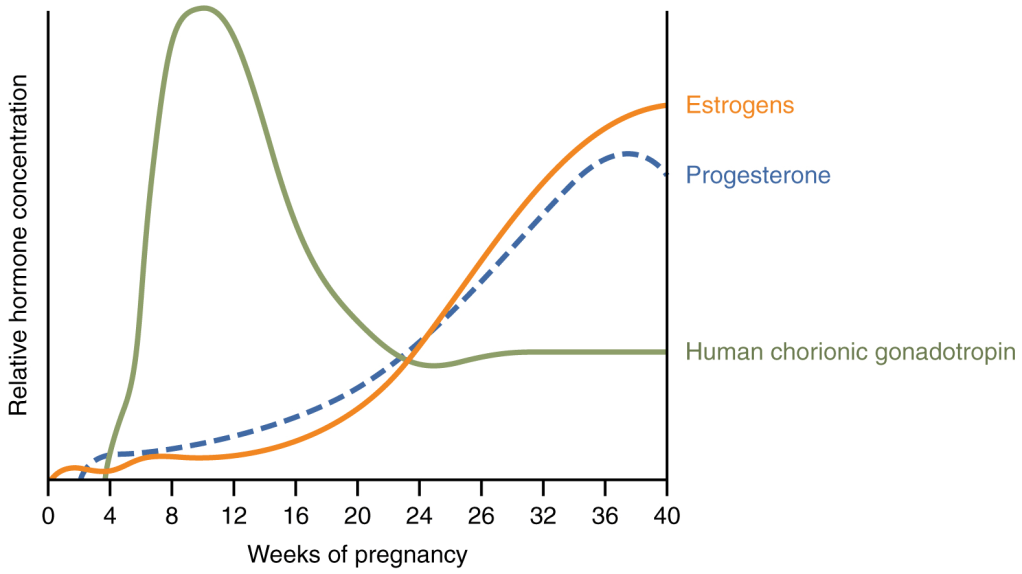
https://chem.libretexts.org/@go/page/499366 3
BABY BLUES
Numerous women experience “baby blues” after giving birth, which is a mild-to-moderate emotional state where mothers experience sadness, mood swings, irritability, and lowered self esteem. Baby blues are a result of the substantial decrease in progesterone and estrogen after birth. These symptoms appear during the first couple days after birth, and they typically resolve within the first couple weeks of new motherhood. Unfortunately, upwards of 70-80% of all new mothers experience this (American Pregnancy Association, n.d.)4. If a mother has a history of depression and anxiety in the past, they are more likely to develop baby blues, as well as other postpartum conditions. It goes without saying that baby blues is usually caused by a combination of factors such as the hormonal changes mentioned previously, the process of physical recovery, emotional stress, sleep deprivation, and more.
POSTPARTUM ANXIETY
Generalized anxiety disorder (GAD) is the most common mental health disorder in the world amongst female populations (Locke et al., 2015)5. Since women are more susceptible to GAD than men, the physical pain and hormonal shifts during pregnancy and labor may increase the chances of developing an anxiety-based condition during recovery. Postpartum anxiety (PPA) is highly undiagnosed. Unlike baby blues, PPA fills mothers with a persistent, overwhelming sense of dread that limits their daily functions for long periods of time. Some of the most common symptoms include 6:
- Overthinking
- Poor appetite
- Mood swings
- Impaired judgment
- Insomnia
- Hair loss
- Panic and anxiety attacks
POSTPARTUM DEPRESSION
Also referred to as “postnatal depression” or “peripartum depression”, this disorder is characterized as a severe and prolonged depressive state that impacts an estimated 1 in 6 mothers in the United States alone (Kroh & Lim, 2021)7. Like PPA, Postpartum Depression prohibits a mother’s daily functions and restricts the ability to regulate emotions and/or properly care for their baby. This misconceived disorder is often confused for baby blues; though both can share similar symptoms, PPD can go beyond the first couple weeks after birth to months, or even years if untreated. Women with postpartum depression are often misdiagnosed by medical professionals and may struggle to receive adequate treatment. Some symptoms of PPD include 8:
- Depressive mood
- Feelings of hopelessness and guilt
- Sadness
- Brain fog
- Emotional and social disconnection
- Irritability and mood swings
- Weight gain or loss
- Appetite issues
- Insomnia
- Suicidal thoughts
POSTPARTUM PSYCHOSIS
Postpartum Psychosis is a rare mental disorder that frequently poses a high risk to both the mother and her baby. Those suffering from this particular psychosis experience severe manic and depressive symptoms that impair the judgement and actions of the mother, often resulting in the endangerment for the mother and her family. Genetic predisposition is regarded as a high contributor to the likelihood of this illness, along with other factors such as physical trauma and intensive hormonal shifts. If a woman lives with borderline personality disorder, bipolar disorder, schizoaffective disorder, or other similar conditions, she may be more likely to develop this. While this condition is relatively rare, especially in the U.S., it still affects an estimated range of 12 million to almost 325 million women globally each year (Cleveland Clinic, n.d.)9. It is extremely scary for mothers, and is declared as a mental health emergency. This requires hospitalization and sometimes counseling for the mother in terms of treatment. It is imperative that the loved ones of someone suffering from PPD should immediately take action and contact emergency services (911) if the mother is suspected to become a threat to herself or others. Some symptoms of postpartum psychosis include 9:
- Impaired judgment
- Severe irritability and anxiety
- Hallucinations
- High paranoia
- Delusions regarding family, friends, and medical professionals
- Dissociation
- Insomnia
- Drastic mood swings
- Suicidal/infanticidal thoughts or actions
Based on the individual, mental disturbances can begin within different stages of motherhood – whether it be uncertainty during pregnancy trimesters, emotional disconnection when holding your baby for the first time, and overwhelming doubt in the postpartum period. The duration of these symptoms is variable as well; some mothers can recover relatively quickly after giving birth, while it could take many years into parenthood to fully heal. Mothers are not the only ones affected by perinatal mood and anxiety disorders, however. Spouses, family, and friends often shoulder the weight of a new mother’s pain. Other factors are known to affect the development and severity of the ailments, such as poor socioeconomic conditions, family and genetic history, financial issues, traumatic pregnancy complications, etc. The external situations a mother is put through may also determine courses of treatment.
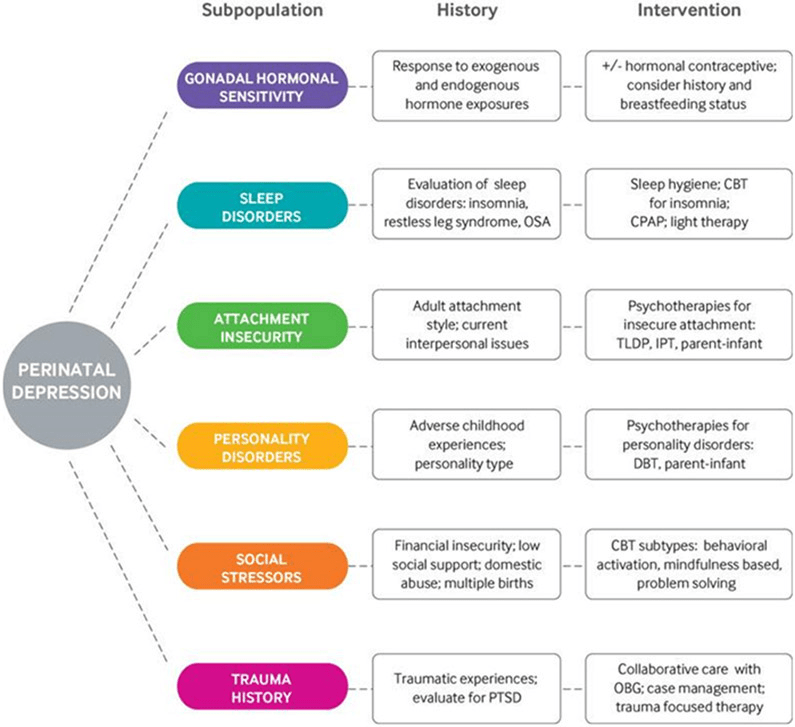
For those suffering, you are not alone, and treatment is always possible. The level of assistance needed is entirely dependent on the person; some mothers may need anti-anxiety/antidepressant medications to help manage symptoms, while others require psychotherapy and counselling. In most cases, women benefit from a measured combination of both. Holistic coping, or at-home treatments, with postpartum mental conditions may look like:
- Reaching out to friends and family
- Joining a support group or seeing a therapist
- Finding ways to rest
- Healthy eating habits
- Exercising in moderation
- Self-care → Finding time for hobbies like reading, crafting, writing, etc.
If possible, mothers should reach out and discuss their feelings and thoughts with an available medical provider. If one does not have access to these means of treatment, immediate help through online websites, support groups, and hotlines may be right for them. Postpartum Support International is the largest platform used to assist mothers and fathers suffering from perinatal mental health struggles by offering current statistics and treatment plans. The number for the PSI hotline is 1-800-944-4773, or can be reached by texting “HELP” to 1-800-944-4773 10
References
- Johns Hopkins Medicine. (2025). “Hormones During Pregnancy.” John Hopkins University. https://www.hopkinsmedicine.org/health/conditions-and-diseases/staying-healthy-during-pregnancy/hormones-during-pregnancy
- Hackenstack Meridian Health. (2023). “What Happens to Your Hormones After Birth?” Hackensack Meridian Health Inc. https://www.hackensackmeridianhealth.org/en/healthu/2023/03/02/what-happens-to-your-hormones-after-birth
- Changes During Pregnancy, Labor, and Birth. (2024, November 7). LibreTexts Chemistry 29: Human Development and Continuity of Life. https://chem.libretexts.org/Workbench/Pick_Your_Poison%3A_Introduction_to_Materials_Toxicology/29%3A_Human_Development_and_the_Continuity_of_Life/29.02%3A_Development_and_Inheritance/29.2.05%3A_Changes_During_Pregnancy_Labor_and_Birth
- American Pregnancy Association Blog. (2025) “Baby Blues” American Pregnancy Association. https://americanpregnancy.org/healthy-pregnancy/first-year-of-life/baby-blues/
- Locke, A. B., Kirst, N., & Shultz, C. G. (2015). “Diagnosis and management of generalized anxiety disorder and panic disorder in adults.” American Family Physician, 91(9), 617–624. https://pubmed.ncbi.nlm.nih.gov/25955736/
- Franciscan Health. (2025, March 27). “Postpartum Anxiety Symptoms: Getting Support”. Franciscan Alliance, Inc. https://www.franciscanhealth.org/community/blog/postpartum-anxiety
- Kroh, S. J., & Lim, G. (2021). Perinatal depression. International Anesthesiology Clinics, 59(3), 45–51. National Library of Medicine. https://pmc.ncbi.nlm.nih.gov/articles/PMC8187301/#S23
- Mayo Clinic Staff. (2022, November 24). “Postpartum Depression”. Mayo Foundation for Medical Education and Research (MFMER). https://www.mayoclinic.org/diseases-conditions/postpartum-depression/symptoms-causes/syc-20376617
- Cleveland Clinic Diseases & Conditions. (Reviewed 2022, September 13). “Postpartum Psychosis”. Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/24152-postpartum-psychosis
- Postpartum Support International. (2025) https://postpartum.net/